
Denials
The average claim denial rate is hovering around 10%, meaning most organizations have millions of dollars of initially denied claims.
Prominence eliminates the majority of the time and money spent on researching, fixing, resubmitting, and collecting on these denied claims.
Root Cause Analysis
Prominence’s Denials Accelerator monitors your organizations denial volumes over time while automatically highlighting variances that require further review. This means your team gets a prioritized list of high-value denials to review, ensuring efficiency. Organizations that have deployed this Accelerator have denial volumes drop by 50%, as preventable denials are identified and upstream fixes applied.
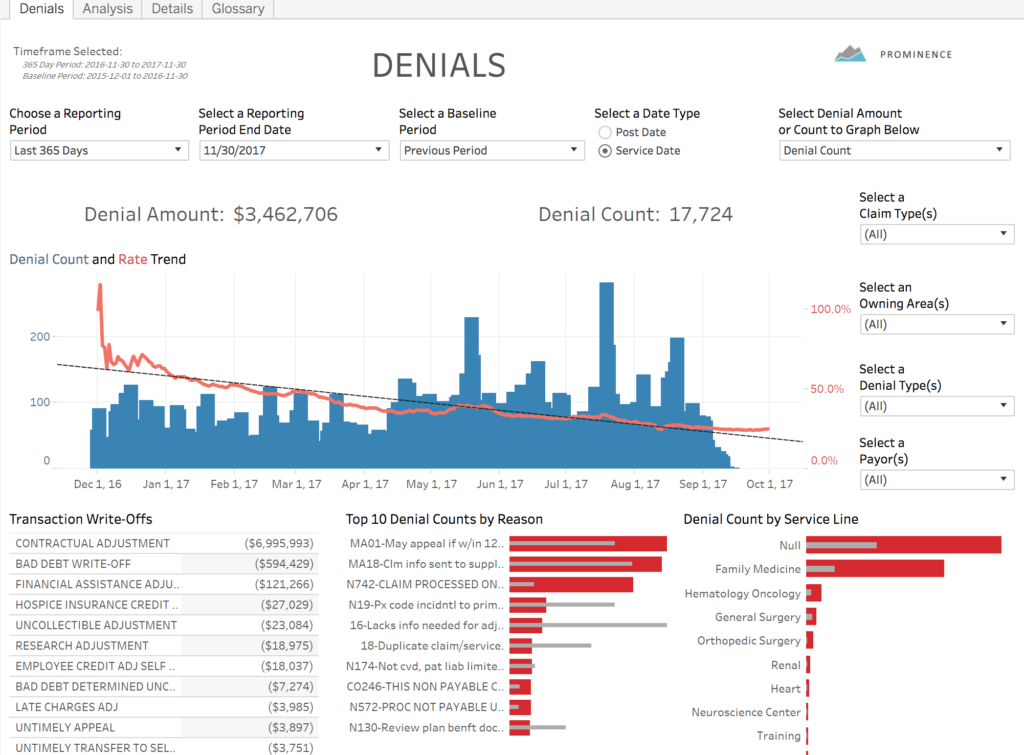
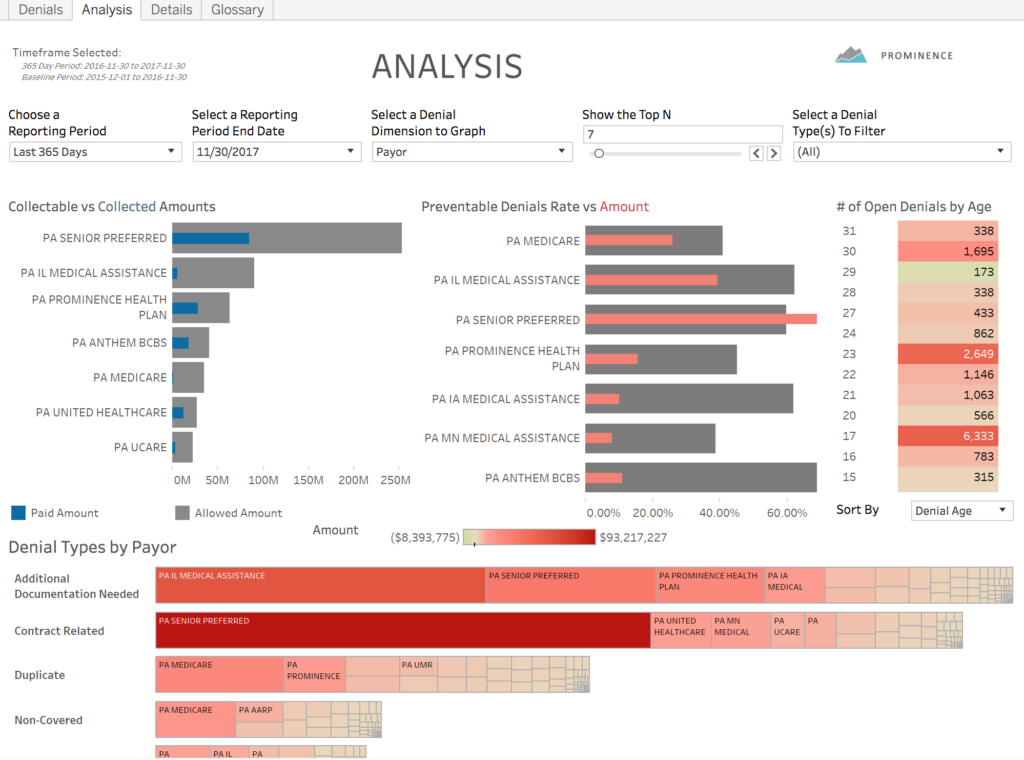
Trusted Data for Everyone
The Denials Accelerator provides a deep-dive into your data, down to row-level details on individual claims, using data from your EHR and payers.
Additionally, each of these metrics is shared globally at your organization, meaning that revenue cycle and finance leaders can view the same key performance indicators in their more broad-ranging dashboards. This keeps everyone on the same page and focused on taking the next best action, instead of arguing over whose number is the ‘right one.’
Prominence Accelerators
Prominence’s Accelerators are pre-built, customizable analytics dashboards that maximize your existing investments in technology and people. The Accelerators leverage data from any source, automate data delivery, and enhance governance without creating untenable maintenance.
- Deliver actionable, governed analytics 4x faster, saving 9 months on average, with the Prominence Platform
- Eliminate 80% of time required to deploy new analytics solutions (800 hours, on average)
- Reduce time required from SMEs by 70% using pre-built content and proven processes (300 hours, on average)
- Don’t recreate the wheel – Prominence’s Accelerators can compliment / enhance your existing analytics or EDW
- Automate data pipelines from source systems and leverage real-time data from Epic, Cerner and other mission critical systems.


